Risks of Colon Cancer in Women and Men
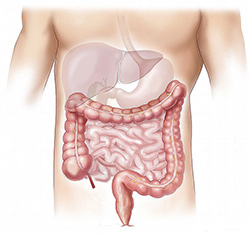 Colon cancer is cancer of the large intestine (colon), the lower part of your digestive system. Most cases of colon cancer begin as small, noncancerous (benign) clumps of cells called adenomatous polyps. Rectal cancer is cancer of the last 6 inches of the colon. Together, they’re often referred to as colorectal cancers.
Colon cancer is cancer of the large intestine (colon), the lower part of your digestive system. Most cases of colon cancer begin as small, noncancerous (benign) clumps of cells called adenomatous polyps. Rectal cancer is cancer of the last 6 inches of the colon. Together, they’re often referred to as colorectal cancers.
Colorectal cancer is the second most common cancer killer overall and third most common cause of cancer-related death in the United States in both males and females.
Who is at risk for colorectal cancer.
Men tend to get colorectal cancer at an earlier age than women, but women live longer so they catch up with men and thus the total number of cases in men and women is equal. Women diagnosed with uterine or ovarian cancer before age 50 are at increased risk of colorectal cancer. Woman with a personal history of breast cancer have only a very slight increase in risk of colorectal cancer. The average age to develop colorectal cancer is 70 years, and 93% of cases occur in persons 50 years of age or older.
You have a higher risk for colon cancer if you have:
- Cancer elsewhere in the body.
- Colorectal polyps
- Crohn’s disease
- Family history of colon cancer
- Personal history of breast cancer
- Ulcerative colitis
.
What are the symptoms of colorectal cancer?
Symptoms of colorectal cancer vary depending on the location of the cancer within the colon or rectum, though there may be no symptoms at all. The most common presenting symptom of colorectal cancer is rectal bleeding. Cancers arising from the left side of the colon generally cause bleeding, or in their late stages may cause constipation, abdominal pain, and obstructive symptoms. On the other hand, right-sided colon lesions may produce vague abdominal aching, but are unlikely to present with obstruction or altered bowel habit. Other symptoms such as weakness, weight loss, or anemia resulting from chronic blood loss may accompany cancer of the right side of the colon.
 If your doctor learns that you do have colorectal cancer, more tests will be done to see if the cancer has spread. Colonoscopy is currently the only test recommended for colorectal cancer screening in average-risk persons at 10 year intervals. Colonoscopic surveillance (also called screening colonoscopy) needs to be available at more frequent intervals for individuals at high risk for colon cancer (for instance, those with a personal history of colorectal cancer or adenomatous polyps; family history of colorectal cancer; non-hereditary polyposis; colorectal cancer; or a pre-disposing condition such as inflammatory bowel disease.
If your doctor learns that you do have colorectal cancer, more tests will be done to see if the cancer has spread. Colonoscopy is currently the only test recommended for colorectal cancer screening in average-risk persons at 10 year intervals. Colonoscopic surveillance (also called screening colonoscopy) needs to be available at more frequent intervals for individuals at high risk for colon cancer (for instance, those with a personal history of colorectal cancer or adenomatous polyps; family history of colorectal cancer; non-hereditary polyposis; colorectal cancer; or a pre-disposing condition such as inflammatory bowel disease.
The first step to avoiding this ailment is prevention with regular tests at the doctor, but there are other ways of getting around this disease in between checkups. Nevertheless, it appears that increasing the fiber content in the Western diet would be useful in the primary prevention of colorectal cancer. It is recommended that physical activity messages promoting at least 30-45 minutes of moderate to vigorous activity on most days of the week be included in primary prevention interventions for cancer. The population prevalence for meeting proposed physical activity criteria for colon cancer prevention is low and much lower than that related to the more generic public health recommendations.
Our bodies need lots of calcium and not only for building strong bones. Colon cancer prevention is one of the most exciting uses for calcium. However, instead of using calcium supplements, this study relied on low-fat dairy products to supply 1,200mg calcium per day. Investigators found this amount of calcium decreased the incidence of changes in the cells lining the colon, which is often seen in the initial stages of colon cancer. A significant protective factor is adequate dietary calcium intake during the period of maximum growth (ages 9 and 25 y), so that proper peak bone mass is achieved by age 20and 30 y and maintained until mid-life, with only slow bone loss in the following years. As already noted, dietary surveys indicate a significant gap between the recommended calcium intake and the actual intake in the United States in the critical years of adolescence and young adulthood and later in life. In addition, several large-scale, recent studies in humans indicate a role for increased dietary calcium in reducing colon cancer risk.
Both men and women are equally at risk for colorectal cancer. Men over the age of 50 and women over 55 should have this test on an annual basis to detect colon cancer early. Yet colorectal cancer is the third most common malignancy in women after breast and lung cancer. Incidence is slightly higher in men than women, and is highest in African American men. It is believed that the time has come for a full scientific review of cereal-grain enrichment with calcium and vitamin D as a low-cost, safe, and useful route for the reduction of osteoporosis and colon cancer in the United States in both men and women.